United Kingdom’s microcredit as a public health initiative
Bridging financial gaps for wellbeing
Case study
United-Kingdom
Microcredit
The UK microcredit initiative uses small, low-interest loans to promote financial inclusion and improve public health. Delivered by socially-oriented lenders like Grameen UK and Scotcash, these loans help individuals on low incomes manage everyday and unexpected expenses, reducing financial stress and supporting wellbeing.
Context and problems addressed
In the UK, health gaps exist and are widening between the best and worst-off in society. These disparities are influenced by social, economic, and environmental factors, and financial exclusion and high-priced debt are associated with worse health. Individuals with low incomes often lack access to affordable financial services, leading them to rely on personal networks, subprime lenders with high interest rates, or cutting back on essentials. These coping mechanisms exacerbate stress, anxiety, and other health issues. The 2007-08 financial crisis led to ‘new geographies of financial exclusion’ being created which affected deprived areas subsequently targeted by exploitative ‘sub-prime’ lenders.
Intervention and financing model
One approach to foster financial inclusion is the provision of microcredits. Microcredits are small loans provided at affordable interest rates to individuals who cannot access traditional banking services due to a lack of collateral and/or credit history.
In the UK, responsible finance providers are the main providers of microcredit. They are different from mainstream lenders – such as banks – because they prioritise the wellbeing and interests of borrowers over profit maximisation, and are lending responsibly. This form of lending is proposed as having potential to act as a public health initiative by impacting on social determinants of health. In Glasgow, two microcredit institutions — Grameen in the UK and Scotcash —provided loans to respectively groups and individuals.
These microloans were designed to reduce financial stress and associated negative mental health outcomes by providing borrowers with resources to meet both expected and unexpected expenses.
The financing model involved low-interest loans provided by socially-oriented institutions. These organisations prioritised the wellbeing of borrowers over profit maximisation, operating with responsible banking practices to prevent over-indebtedness. This included thorough affordability checks and flexible repayment terms that were adjusted to suit the borrower’s financial situation.
The financing model involved low-interest loans provided by socially-oriented institutions. These organisations prioritised the wellbeing of borrowers over profit maximisation, operating with responsible banking practices to prevent over-indebtedness.
Key outcomes and associated measurements
Findings of a study evaluating the microcredit intervention in Glasgow found that microcredits had mixed outcomes. On one hand, loan use was perceived as impacting positively on health and wellbeing outcomes, including control, confidence, feeling of self-worth, positive mental health, and social participation. Access to flexible, responsibly delivered, loans helped participants feel less marginalised, enabling them to plan and feel secure when faced with (un)expected financial events. On the other hand, some borrowers experienced stress due to the obligation of repaying the loans, particularly those on very low incomes.
While microcredit programmes may not be inherently profitable for financial institutions, systemic support such as subsidies or frameworks like the Community Reinvestment Act can incentivise responsible finance providers to continue offering these services, ensuring they remain accessible to vulnerable populations while delivering social benefits.
Related case studies
Tackling inequality among children and young people in UK’s West London Zone
Fair chance fund
ADIE’s social impact contract
About EuroHealthNet
Building a healthier future for all by addressing the determinants of health and reducing inequalities.
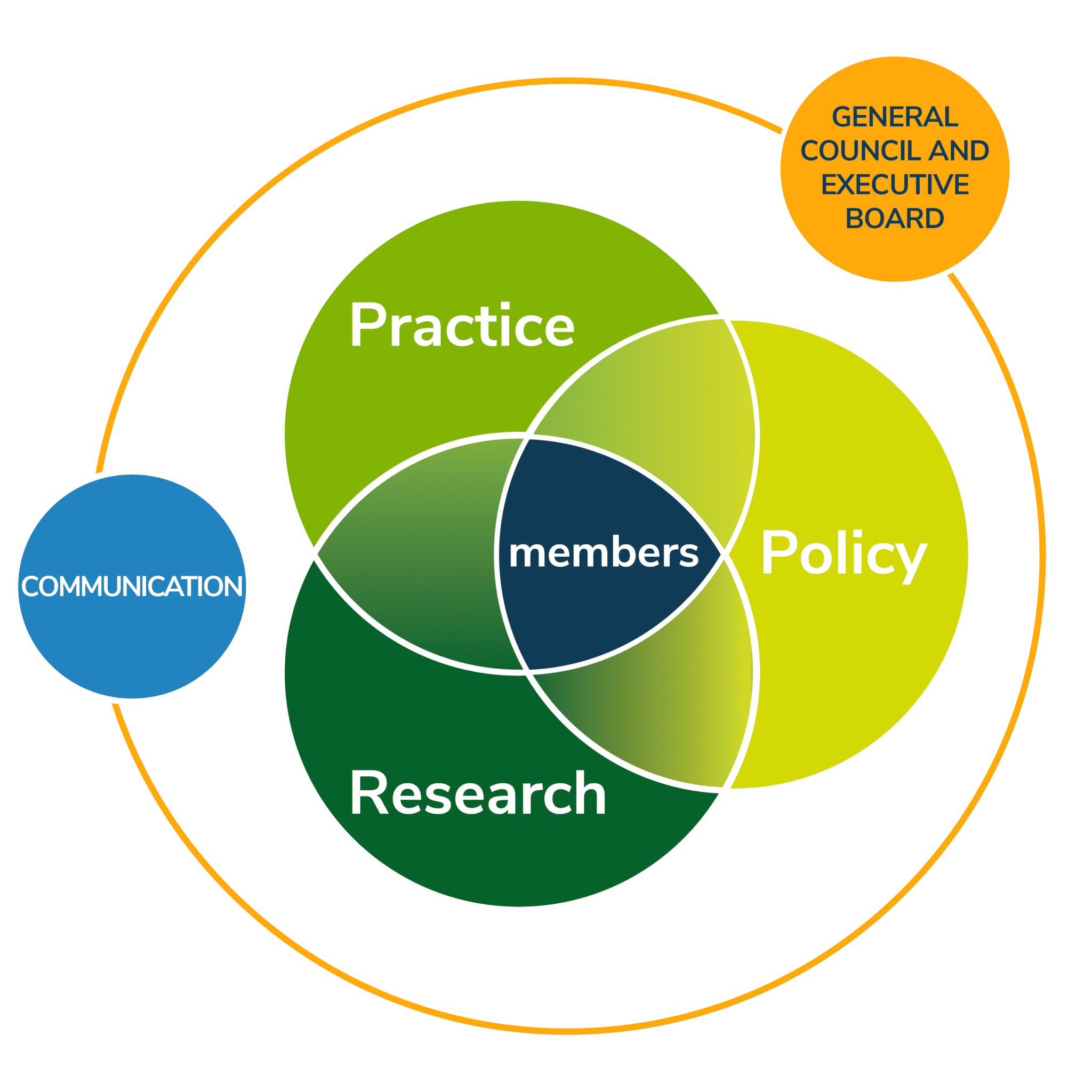
EuroHealthNet is the Partnership of public health agencies and organisations building a healthier future for all by addressing the determinants of health and reducing inequalities. Our focus is on preventing disease and promoting good health by looking within and beyond the health system.
Structuring our work over a policy, a practice, and a research platform, we focus on exploring and strengthening the links between these areas.
Our approach focuses on integrated concepts to health, reducing health inequality gaps and gradients, working on determinants across the life course, whilst contributing to the sustainability and wellbeing of people and the planet.

EuroHealthNet is co-funded by the European Union. However, the information and views set out on this website are those of the author and do not necessarily reflect the official opinion of the European Commission. The Commission does not guarantee the accuracy of the data included on this website. Neither the Commission nor any person acting on the Commission's behalf may be held responsible for the use which may be made of the information contained therein.